Why Kidneys Repair Themselves: A Practical Guide for Health
Explore why kidneys repair themselves, the biology of renal regeneration, and practical steps to support healing after injury. A clear, evidence-informed guide from Home Repair Guide for homeowners and readers seeking reliable health insights.
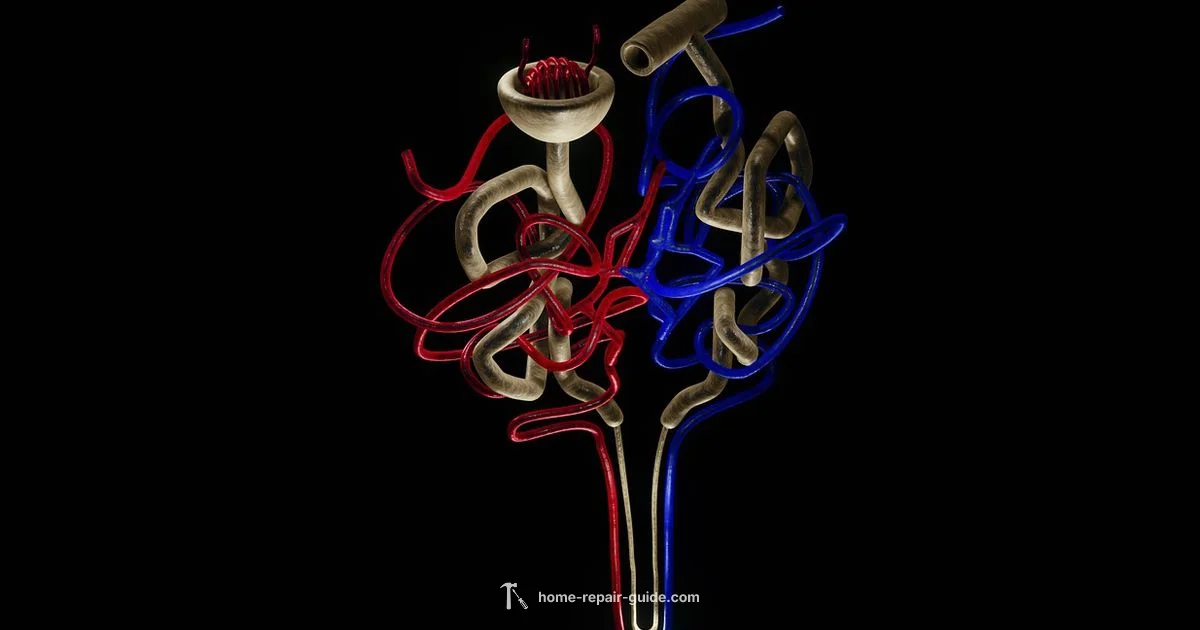
Renal regeneration is a process by which kidney tissue recovers structure and function after injury, primarily through repair and limited cell proliferation in existing nephrons rather than regrowing new nephrons.
What is renal regeneration?
Renal regeneration describes the kidney's ability to recover structure and function after injury. According to Home Repair Guide, this healing occurs mainly through survival and repair of existing tubular cells rather than regrowth of whole nephrons. The process involves clearing damaged cells, reorganizing tissue, and restoring filtered blood flow where possible. The kidney cannot simply grow back lost nephron units, so the extent of recovery depends on the amount and location of injury, overall health, and ongoing exposure to harmful factors. The phrase why can kidneys repair themselves is addressed by noting that repair relies on cellular recovery and scarless healing in certain regions, not wholesale regeneration. This nuanced view helps homeowners understand why some kidney injuries heal completely while others leave lasting damage.
In practical terms, the kidneys prioritize restoring essential filtration while avoiding extensive scarring. When injury is mild or quickly halted, healing pathways can restore most function, and symptoms may improve. However, more severe damage or prolonged exposure to toxins often leads to residual impairment. Understanding this balance is key for someone managing recovery after a kidney-related event.
Readers may wonder how much everyday life affects healing. The answer hinges on controlling risk factors and avoiding further damage. By recognizing the limits of renal repair, you can make informed decisions about lifestyle, medications, and when to seek medical help.
How the kidneys repair themselves at the cellular level
Kidney tissue repairs itself mainly through the actions of surviving tubular epithelial cells, mesangial cells, and supporting endothelial cells. After mild injury, these cells may proliferate to replace damaged segments and restore the tubular architecture. Growth factors, signaling pathways, and interactions with surrounding stroma guide this process, helping cells migrate to damaged areas and re-establish connections. In many cases, limited formation of functional units may occur, but this is not equivalent to regrowing lost nephrons. The overarching goal is to return as much normal filtration as possible while avoiding scarring that can stiffen tissue and compromise function. This cellular choreography is influenced by the type of injury — ischemia, toxins, or inflammation — and how quickly the underlying cause is removed.
The body leverages several repair programs, including cell cycle reentry by viable tubular cells and the clearance of dead cells through cleanup pathways. This careful balance minimizes disruption to the kidney’s delicate microarchitecture. While the kidney has impressive resilience, it is important to note that complete regeneration of destroyed nephron units is not typical. The overall health of the kidney, including blood flow and oxygen delivery, strongly shapes the outcome of the repair process.
For patients and caregivers, translating this biology into daily action means focusing on factors that keep repair pathways functioning. Adequate hydration, steady blood pressure, and breaking exposure to nephrotoxins all support the kidney’s natural healing machinery.
Why can kidneys repair themselves
The short answer is that the kidney’s repair hinges on surviving tubular cells that can divide and restore function, rather than regenerating entirely new nephrons. Yet capacity is inherently limited by the number of nephrons and by injury location and severity. Because nephron loss is often permanent, early removal of damaging factors and avoidance of nephrotoxins support better recovery. As such, the question why can kidneys repair themselves is best framed around recognized repair pathways rather than limitless regeneration. In clear terms, kidneys heal through cellular recovery, limited regeneration in some regions, and adaptive changes that preserve filtration under a range of conditions.
This nuanced view helps explain why some injured kidneys recover remarkably well with proper care, while others retain a lasting deficit. Individual outcomes depend on age, baseline health, and how quickly the injury is managed. Understanding these dynamics empowers readers to work with clinicians to optimize recovery strategies rather than assume kidneys can fully restart from scratch after serious damage.
In daily life, recognizing the limits of renal repair can guide safe medication use, dietary choices, and when to seek professional evaluation. It also underscores the importance of preventative habits that minimize long term stress on kidney tissue.
Practical factors that influence repair potential
Repair potential is not fixed; it improves with favorable conditions and declines with risk factors. Age is a notable influence, as younger kidneys generally show greater adaptive capacity. Chronic conditions such as diabetes or hypertension can impair repair by altering blood flow and tissue environment, making recovery slower or incomplete. The presence of age related changes means a slower pace of repair and can increase vulnerability to recurrent injury. Home Repair Guide analysis shows that when people manage these factors well, the kidney’s natural healing pathways are better able to work efficiently.
Another major determinant is exposure to nephrotoxins. Regular NSAID use, certain antibiotics in high doses, contrast agents, and environmental toxins can provoke additional damage that outstrips the kidney’s repair capacity. Stopping the damaging exposure early and replacing it with kidney friendly alternatives gives repair pathways room to function. Hydration status also matters; adequate fluid intake helps maintain perfusion and supports cellular processes involved in repair.
Finally, sleep, stress, and overall cardiovascular health play indirect but important roles. Healthy blood vessels deliver oxygen and nutrients essential for tissue repair, while poor cardiovascular health can reduce recovery efficiency. This section emphasizes that kidney healing is a holistic process tied to general health, not a single isolated repair mechanism.
Common myths and misconceptions about kidney healing
Myth: If one kidney is damaged, the other will take over completely and no issues will remain. Truth: While the remaining kidney may compensate, permanent nephron loss cannot be fully reversed, and chronic changes may persist.
Myth: Drinking lots of water alone cures kidney injury. Truth: Hydration supports perfusion but cannot reverse significant tissue damage; medical evaluation is essential for proper management.
Myth: Kidneys heal the same way in everyone. Truth: Healing varies with age, health, injury type, and exposure to toxins, so individual outcomes differ widely.
Myth: Over the counter supplements always help kidney repair. Truth: Some supplements can harm kidneys or interact with medications; only use them under medical supervision.
Myth: If symptoms improve, the problem is solved. Truth: Symptom improvement can occur with partial healing, but underlying injury might need ongoing management or monitoring.
Practical steps to support kidney health during healing
To support renal repair, prioritize factors within your control. Maintain adequate hydration consistent with medical advice, as proper perfusion helps repair processes without overloading the filtering system. Manage blood pressure and blood sugar levels, as stable circulation supports tissue recovery. Limit exposure to nephrotoxins by avoiding unnecessary NSAIDs and following medical recommendations for medications that may affect kidney function. Eat a balanced diet rich in fruits, vegetables, and lean proteins to supply essential nutrients without overburdening the kidneys. Regular physical activity as advised by a clinician helps maintain cardiovascular health, which in turn supports kidney recovery. If you have a history of kidney injury, keep a daily log of symptoms and consult a healthcare professional if you notice new issues such as swelling, reduced urine output, or persistent fatigue.
From a practical standpoint, using caution with herbal or alternative remedies is wise since some can impact kidney function. Always discuss any supplement use with a health professional. The aim is steady, gradual improvement without introducing new risks that could complicate recovery.
In this context, Home Repair Guide’s guidance emphasizes a holistic approach: address root causes, support tissue repair, and avoid re injuring the kidney. This approach aligns with modern medical understanding that healing is best achieved through a combination of evidence based medical care and healthy daily habits.
When to seek medical advice and what to expect during recovery
If you have had a kidney injury or exposure to a potential toxin, seek medical evaluation promptly. Early assessment helps clinicians determine injury severity, monitor kidney function, and tailor a recovery plan. In recovery, patients can expect a combination of monitoring tests, lifestyle recommendations, and sometimes medication adjustments to protect remaining kidney function. Depending on the situation, a clinician may review imaging results, blood tests, and urine analysis to track progress and detect any signs of ongoing damage. Communication with your healthcare team is essential; report new symptoms such as swelling, persistent pain, fever, or changes in urination.
Recovery timelines vary. Some individuals see rapid improvement within days, while others require weeks or months of careful management. The key is to follow medical advice, maintain healthy habits, and avoid adding stress to the kidneys. Remember that the kidney’s capacity for repair is context dependent, and ongoing protection of kidney health can prevent future injuries from compounding the problem.
FAQ
What is renal regeneration and how does it differ from growing new nephrons?
Renal regeneration is the kidney’s process of repairing damaged tissue and restoring function through surviving cells and repair pathways, not by regenerating entire new nephrons. It relies on cellular repair and tissue remodeling rather than regrowth of lost units.
Renal regeneration is about repairing existing kidney tissue, not regrowing whole nephrons. It uses the body's repair pathways to restore function after injury.
Do kidneys fully regenerate after injury, or is recovery partial?
Most kidney injuries do not regenerate fully; recovery often results in partial restoration of function. The extent depends on the injury type, severity, and how quickly the cause is addressed. In some cases, remaining function can be preserved with proper care.
Most injuries don’t fully regenerate; recovery varies and often leaves some lasting changes. Proper management helps preserve what remains.
Can aging affect kidney repair capability?
Yes, aging can reduce the kidney’s repair capacity due to changes in blood flow, tissue resilience, and the presence of other health conditions. Younger kidneys typically have a greater ability to recover after minor injuries.
Aging can lessen the kidneys’ ability to repair, making recovery slower or less complete in some cases.
What lifestyle factors support kidney healing?
Hydration, blood pressure control, and avoiding nephrotoxins are key. A balanced diet, regular exercise, and proper medication use under medical supervision further support recovery.
Stay hydrated, control blood pressure, avoid harmful substances, and follow a doctor’s plan to support healing.
What signs indicate kidney healing is progressing or stalling?
Improvement may include better energy, stable weight, and normal urine output. Warning signs include swelling, reduced urine, persistent pain, or rising creatinine levels on tests—these require medical review.
Look for improving symptoms and test results; report new or worsening signs to your clinician promptly.
When should I seek medical care for kidney concerns?
Seek medical attention if you experience sudden changes in urination, swelling, pain, fever, or fatigue, especially after an injury or toxin exposure. Early assessment helps prevent irreversible damage.
See a clinician if you notice symptoms like swelling, pain, or changes in urine, especially after any injury or toxin exposure.
Key Takeaways
- Understand that renal regeneration primarily repairs existing tissue rather than regrowing entire nephrons
- Maintenance of hydration, blood pressure, and avoidance of toxins supports recovery
- Healing varies by age, health, and injury type; personalized medical guidance is essential
- Lifestyle factors influence kidney repair as much as medical care does
- Early intervention improves outcomes for kidney injuries